Abstract
Objectives: The National Report Card on Osteoporosis Care (2008) announced the need for comprehensive approaches to risk reduction and improvement in the early diagnosis of osteoporosis. Dental research has suggested that low systemic bone-mineral density also occurs in alveolar bone, and people with osteoporosis may have an increased risk of tooth loss. Whether or not a causal link exists, both conditions share similar modifiable risk factors, including a role for calcium and vitamin D. The purpose of this paper was to critically examine the role calcium and vitamin D play in the relationship between osteoporosis and the risk of tooth loss.
Methods: Scientific articles were obtained through PubMed, MEDLINE, CINAHL, AgeLine and Web of Science. Publications were restricted to those involving human subjects, and English-language articles on calcium and vitamin D. The search yielded 8 articles relating to osteoporosis and tooth loss that included calcium and vitamin D intake.
Results: Despite methodological concerns, the evidence shows a relationship between osteoporosis and tooth loss for people who have an inadequate intake of calcium and vitamin D. Adequate calcium intake positively influences optimal peak bone mass and may also assist in tooth retention in later life.
Conclusions: The dental sector can assist with national prevention strategies for osteoporosis care.
Introduction
Canadian statistics indicate that 2 million people are currently diagnosed with osteoporosis.1 Because of its impact on both people individually2-4 and the health care system,5,6 osteoporosis is recognized as a major public health concern.7 Despite the pervasiveness of osteoporosis and its consequences for the Canadian population, statistics continually indicate long-standing difficulties with access and referral to screening for bone-mineral density.8 Consequently, new priorities for osteoporosis care need to be established.1 These priorities include the improvement of early diagnosis and the development of comprehensive approaches to risk reduction.8
Optimizing peak bone mass achieved during adolescence and young adulthood is one crucial component of reducing the risk of osteoporosis in later life.7 Adequate consumption of calcium and vitamin D is critical to the achievement of optimal peak bone mass.8 Prolonged inadequate consumption of calcium stimulates bone resorption, which leads to systemic bone fragility.9 Unfortunately, many Canadians are not consuming adequate amounts of calcium throughout their lifespan to achieve and maintain optimal peak bone mass.
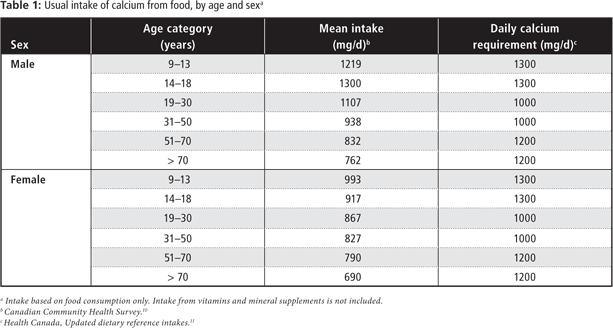
As Table 1 shows, women's mean calcium intake from food is considerably lower than the recommended intake across all ages.10,11 Although younger men tend to consume adequate amounts of calcium to achieve optimal peak bone mass, as they age, fewer consume the recommended amount of calcium to maintain their bone-mineral density. Consequently, interventions for osteoporosis prevention have included improving calcium intake throughout the lifespan.7
Relationship between Osteoporosis and Tooth Loss
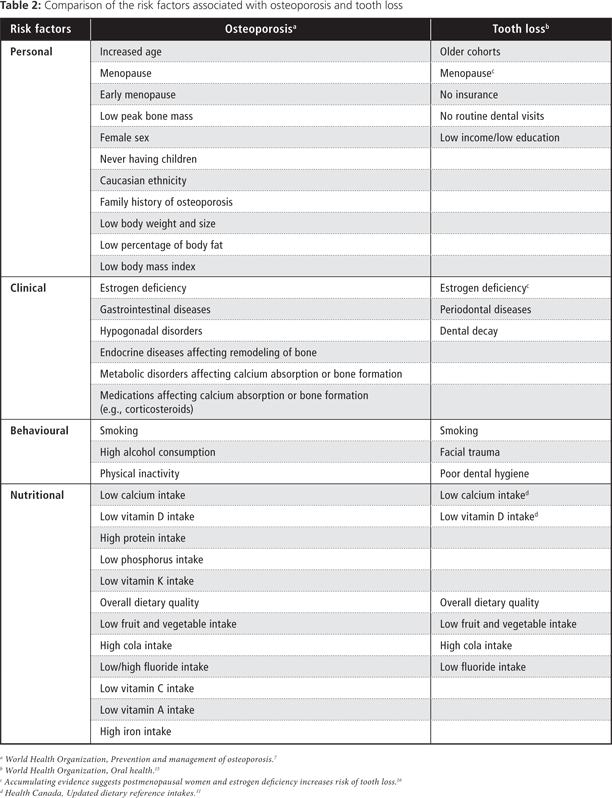
The dental sector has a potential role in the early detection of osteoporosis.12 Early research14 suggested that low systemic bone-mineral density also occurs in alveolar bone13 and hypothesized the risk of tooth loss. However, a causal association between these 2 conditions may never be established. Both osteoporosis and tooth loss are multifactorial conditions (Table 2) that have many unique and shared risk factors.7,11,15,16 Many of these shared risk factors are modifiable, including the adequate intake of calcium and vitamin D.7,11
Further, the literature describes many factors that may play mediating roles between oral health and systemic diseases. Ritchie and colleagues17 discussed how oral health can affect nutritional intake and, in turn, how poor nutrition can play a role in systemic disease. The supportive role calcium and vitamin D play in bone resorption could explain the link between osteoporosis and the risk of tooth loss. Traditional interventions for tooth retention (e.g., dental hygiene) might not be sufficient for people with a diagnosis of osteoporosis.18 Additional interventions for the maintenance of optimal peak bone mass, including calcium and vitamin D supplementation, may also be beneficial for tooth retention. Evaluating the role of calcium and vitamin D in this relationship may provide insight into the development of early interventions.
The purpose of this literature review was to examine the role of calcium and vitamin D intake in the relationship between osteoporosis and tooth loss, and to provide an evidence base for the role dental professionals should play in supporting strategies for preventing osteoporosis in clinical practice.
Methods
Scientific articles were obtained through PubMed, MEDLINE, CINAHL, AgeLine and Web of Science. The following Medical Subject Headings were used: "osteoporosis," "tooth loss" and "edentulous." Publications were restricted to those about human subjects and English-language articles. All articles obtained covered the publication period from 1983 to 2011. Review articles and reference lists were examined for relevance to the topic. All articles were then reviewed for their consideration of calcium and vitamin D intake.
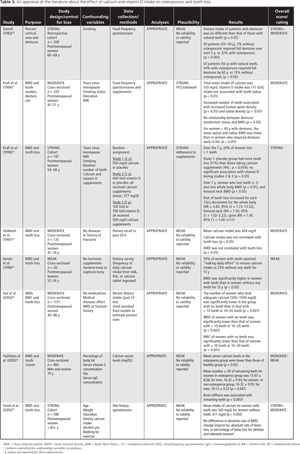
Eight studies that considered the role of calcium or vitamin D, or both, in the relationship between osteoporosis and tooth loss were identified. An appraisal of all 8 studies was subsequently completed. The strength of the evidence in the studies was evaluated based on sample size and representativeness, confounding factors, and methods of data collection and analyses. Evaluation of the plausibility of findings was based on the evaluations or pilot testing of the calcium and vitamin D measures. Both strength of evidence and plausibility were used to identify studies as weak, moderate or strong.19 An overview these 8 studies is presented in Table 3.
Results
Of the 8 studies, 3 were cohort studies20,22,26 and the remaining 5 were cross-sectional.18,21,23-25 All 8 studies used techniques to measure low systemic bone-mineral density. Five studies18,21,22,24,26 used dual-energy x-ray absorptiometry, widely accepted as the gold-standard technique for measuring bone-mineral density.7 Hence, the majority of these studies used actual measures of bone-mineral density to ascertain a diagnosis of osteoporosis.
Tooth loss was measured by denture status,20 tooth counts during examinations,21,25 dental radiographs,23 self-reported tooth loss18,22,24 or being completely edentulous.26 Earlier studies were criticized for including people with missing teeth because of traditional dental extractions.14 Assessing the underlying reason (e.g., no trauma) is necessary to rule out tooth loss that is not likely related to resorption from supporting bone. Although radiographs and tooth counts done during dental examinations likely take into account the reasons for tooth loss (e.g., progressive alveolar bone loss, periodontal diseases) the underlying reasons for tooth loss were unknown in all studies. These methods of ascertaining tooth loss cannot, therefore, fully support or refute a hypothesis that tooth loss was the result of alveolar-bone resorption caused by low systemic bone-mineral density.
Sample Representativeness
All of the study samples included older postmenopausal women. Only 1 study25 included a sample of both older women and men. This suggests that these findings can be generalized only to older postmenopausal women. Indeed, Earnshaw and colleagues27 found no association between tooth loss and low systemic bone-mineral density in younger early menopausal age groups (e.g., women < 50 years of age). Older-age cohorts have higher rates of tooth loss15 because of early dental treatment procedures as children (e.g., tooth extractions), which may partially explain tooth loss in older cohorts when reasons are unknown. However, given the importance of the estrogen hormone to the balance between bone resorption and formation,28 these findings may have additional implications for preventive interventions for women, which are discussed later in this paper.
Calcium and Vitamin D Intake
Consistent with Canadian population data, a trend toward low calcium intake was noted in all studies reviewed. All 8 studies reported mean calcium intakes ranging from 500 to 1000 mg per day. The recommended average intake of calcium for women ≥ 51 years of age is 1200 mg daily.11 Only 2 identified studies21,22 considered vitamin D intake. Again, participants in these studies consumed less than recommended dietary intakes for vitamin D (111–700 IU/day versus adequate intakes of 600–800 IU/day). This suggests that, on average, participants were not consuming adequate amounts of calcium to ensure optimal bone and dental health.
Measurement of Calcium and Vitamin D Intake
Measurement of calcium intake included food frequency questionnaires,20,21,24 dietary recall,23 recent dietary intakes,18 serum calcium levels,25 supplementation21,22 and diet history questionnaires.26 Only 2 studies assessed vitamin D and tooth loss, both with supplementation.21,22 However, Krall and colleagues21 supplemented these data with information about habitual vitamin D intake obtained from food-frequency questionnaires.
Although these assessments provide an estimate of current dietary intake, they may not accurately represent intake across the lifespan. Studies that record daily intake of calcium based on 24-hour recalls are not likely sufficient to describe participants' usual intake of calcium.29 Although food-frequency questionnaires are considered sufficient for approximating the usual dietary intake of populations over the period in question, multiple dietary-intake measures to support the validity of the dietary information are needed.29 Also, not all of these studies indicated whether participants were taking supplements in addition to current dietary intake of vitamin D or calcium, an important factor to assess when considering intake. These studies did not use robust measures or multiple measures to provide a more complete picture of current and habitual intake of vitamin D and calcium.
Analyses and Confounding Variables
Famili and colleagues26 found a significant relationship (p = 0.002) between dietary history of calcium intake and edentate postmenopausal women. The finding of the cohort study of Krall and colleagues22 that postmenopausal women in the placebo group had more tooth loss than those taking calcium supplementation over a 2-year period approached significance (p = 0.05). No significant association was found between vitamin D supplementation and tooth retention.21,22 The measure used to estimate calcium intake likely explains these findings. Nevertheless, since vitamin D is essential to bone health,7 ensuring that participants consume adequate amounts of both calcium and vitamin D across the lifespan is prudent.
Overall, all 8 studies reported low calcium or vitamin D intake, and all but 2 studies found an association between osteoporosis and tooth loss.21,22 In their cross-sectional study, Hildebolt and colleagues23 reported nonsignificant findings; however they acknowledged that their participants were in good dental and overall health, which may have influenced their ability to detect an association. Moreover, despite reporting low calcium intake, all their postmenopausal study participants were taking estrogen replacement therapy, which, given the significant effect of the estrogen hormone on bone,28 may have affected the ability to detect a significant association.
The strongest evidence in the studies that included a measure of effect of calcium and vitamin D intake on the relationship between osteoporosis and tooth loss came from 3 cohort study designs20,22,26 (Table 3). Only 2 of these studies20,22 found a relationship between osteoporosis and tooth loss. The retrospective study by Daniell20 suggested an association between osteoporosis and the need for full dentures in a sample of postmenopausal women. Although these findings are statistically significant, denture status cannot be used to indicate that patients with osteoporosis also had an increased risk of tooth loss.
The remaining 2 cohort studies22,26 included calcium intake as a confounding variable and measured calcium intake differently.
Krall and colleagues22 investigated tooth retention and low systemic bone-mineral density in a cohort study of postmenopausal women who were receiving calcium and vitamin D supplementation. Despite good adherence, postmenopausal women who lost teeth had consistently unfavourable patterns of systemic bone-mineral density change compared with women who retained their teeth. The authors observed that women who were taking the placebo lost more teeth than those women taking calcium supplementation. This study found no significant association between vitamin D intake and tooth loss.
In their cohort study, Famili and colleagues26 found no significant differences in age-adjusted bone-mineral density and absolute rates or percentages of bone loss between dentate and edentate participants after adjusting for a history of dietary calcium intake. Dentate participants had a higher intake of calcium and a higher bone-mineral density than edentate participants.
These last 2 studies22,26 together support a hypothesis that an inadequate intake of calcium plays some role in causing osteoporosis and tooth loss. This suggests a possible mediating role for adequate lifetime calcium or vitamin D intake in the prevention of osteoporosis and tooth loss. An imbalance in bone resorption may also increase the risk of tooth loss when people do not consume adequate amounts of calcium throughout their lifespan. Ensuring that people with low systemic bone-mineral density have adequate amounts of calcium also may improve tooth retention.14
Discussion
Relevance to Dental Practice
This literature review critically examined the role calcium and vitamin D intake plays in the relationship between osteoporosis and tooth loss. Regardless of the true causal association, the studies reviewed suggest that ensuring a lifelong adequate dietary intake of calcium and vitamin D would help to support good bone and dental health. Dental professionals should, therefore, assist in the achievement and maintenance of optimal peak bone-mineral density in their clinical practices.
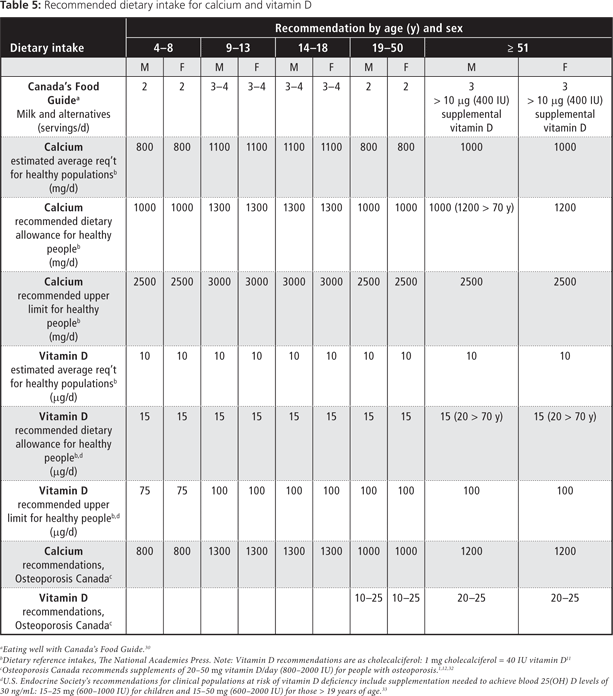
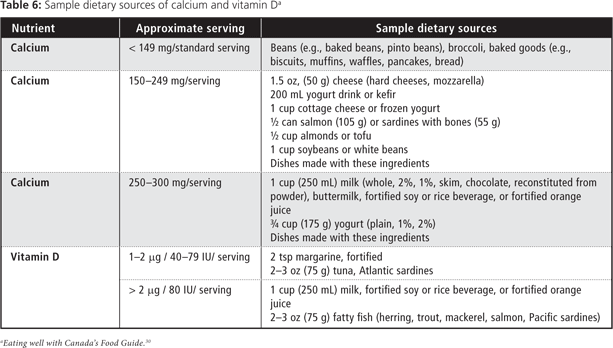
Data from the Canadian Community Health Survey, 2005 indicates that children and young adults are likely to visit dental professionals more frequently than medical physicians (Table 4). Consequently, optimal peak bone-mineral density is achieved during the time when Canadians are likely regularly attending dental offices. Given this trend, dental professionals have an opportunity to regularly discuss osteoporosis prevention with their patients. Creating an awareness of the importance of achieving and maintaining optimal peak bone mass during regular scheduled dental appointments could help prevent osteoporosis and ensure overall dental health. Table 5 provides the recommended dietary intake of calcium and vitamin D1,11,30-33 and Table 6, examples of dietary sources that dental professionals can discuss with their patients.

Early evidence from randomized control trials indicates that calcium and vitamin D supplementation may aid in tooth retention in early menopausal women.30 Given the association between menopause and tooth loss, dental professionals should regularly discuss the importance of adequate dietary calcium and vitamin D consumption (e.g., the need for supplementation) throughout their patients' lifecycle.
Finally, Osteoporosis Canada1 recommends that all postmenopausal women and men ≥ 65 years of age be tested for osteoporosis. Edwards and Migliorati12 suggested that medical and dental professionals could collaborate in the early detection of osteoporosis. Since osteoporosis may first occur in alveolar bone,13 dental professionals may be able to provide early detection of low systemic bone-mineral density and assist medical professionals in identifying people at risk for osteoporosis. One method identified is to increase the number of discussions of these risks with patients during scheduled dental radiographs and examinations. Dental patients who have reduced alveolar bone but good dental hygiene may need further screening for systemic bone-mineral density.18 Referrals to their medical professionals to discuss these findings may further identify those people with low systemic bone-mineral density. Collaboration between professions may help increase the number of people who receive an early diagnosis of osteoporosis.
Conclusions
This review of the literature highlights the role of calcium and vitamin D intake in, and the similar risk factors for, osteoporosis and tooth loss, regardless of their cause. Dental professionals could help patients achieve and maintain hygiene may indicate the need for further systemic bone-mineral density screening.
THE AUTHORS
References
- Osteoporosis Canada. Focus on fractures: Osteoporosis Canada launches new clinical practice guidelines. Toronto, ON: Osteoporosis Canada; 2011. Available: www.osteoporosis.ca/index.php/ci_id/10159/1a_id/1.htm (accessed 2012 Mar 2).
- Nevitt MC, Ettinger B, Black DM, Stone K, Jamal SA, Ensrud K, et al. The association of radiographically detected vertebral fractures with back pain and function: a prospective study. Ann Intern Med. 1998;128(10):793-800.
- Keene GS, Parker MJ, Pryor, GA. Mortality and morbidity after hip fractures. BMJ. 1993;307(6914):1248-50.
- Schroder HM, Petersen KK, Erlandsen M. Occurrence and incidence of the second hip fracture. Clin Orthop Relat Res. 1993;289:166-9.
- Johnell O, Oden A, Caulin F, Kanis JA. Acute and long-term increase in fracture risk after hospitalization for vertebral fracture. Osteoporos Int. 2001;12(3):207-14.
- Leibson C, Tosteson A, Gabriel S, Ransom JE, Melton LJ. Mortality, disability, and nursing home use for persons with and without hip fracture: a population-based study. J Am Geriatr Soc. 2002;50(10):1644-50.
- World Health Organization. Prevention and management of osteoporosis: report of a WHO scientific group. WHO technical report series; 921. Geneva, Switzerland: World Health Organization Scientific Group on the Prevention and Management of Osteoporosis; 2003. Available: http://whqlibdoc.who.int/trs/WHO_TRS_921.pdf. (accessed 2012 Mar 2).
- Osteoporosis Canada. Breaking barriers not bones: 2008 national report card on osteoporosis care. Toronto, ON: Osteoporosis Canada. Available: www.osteoporosis.ca/multimedia/images/english/home/2008NationalReportCard_Eng.pdf (accessed 2012 Feb 16).
- Heaney RP, Weaver CM. Newer perspectives on calcium nutrition and bone quality. J Am Coll Nutr. 2005;24(6 Suppl):574S-81S.
- Statistics Canada. Canadian Community Health Survey, Cycle 2.2, Nutrition (2004), Nutrient Intakes from Food: Provincial, Regional and National Summary Data Tables, Volume 1,2 and 3 [internet]. Ottawa, ON: Health Canada. Available: www.hc-sc.gc.ca/fn-an/surveill/nutrition/commun/cchs_focus-volet_escc-eng.php#p1 (accessed 2012 Feb 16).
- Health Canada. Dietary reference intakes. Ottawa, ON: Health Canada. Available: www.hc-sc.gc.ca/fn-an/nutrition/reference/index-eng.php(accessed 2012 Feb 16).
- Edwards BJ, Migliorati CA. Osteoporosis and its implications for dental patients. J Am Dent Assoc. 2008;139(5):545-52.
- Manzke E, Chestnut CH 3rd, Wergedal JE, Baylink DJ, Nelp WB. Relationship between local and total bone mass in osteoporosis. Metabolism. 1975;24(5):605-15.
- Tooth loss linked to osteoporosis. J Am Dent Assoc. 1994;125(8):1058.
- World Health Organization. Oral health. Geneva, Switzerland: World Health Organization; 2012. Available: www.who.int/oral_health/en/ (accessed 2012 Feb 16).
- Buencamino MC, Palomo L, Thacker HL. How menopause affects oral health, and what we can do about it. Cleve Clin J Med. 2009;76(8):467-75.
- Ritchie CS, Joshipura K, Hung HO, Douglass CW. Nutrition as a mediator in the relation between oral and systemic disease: associations between specific measures of adult oral health and nutrition outcomes. Crit Rev Oral Biol Med 2002;13(3):291-300.
- Gur A, Nar K, Kayhan O, Atay M, Akyuz G, Sindal D, et al. The relation between tooth loss and bone mass in postmenopausal osteoporotic women in Turkey: A multicenter study. Journal Bone Mineral Metabolism. 2003;21:43-7.
- Cameron R, Jolin MA, Walker R, McDermott N, Gough M. Linking science and practice: toward a system for enabling communities to adopt best practices for chronic disease prevention. Health Promot Pract. 2001;2(1):35-42.
- Daniell HN. Postmenopausal tooth loss. Contributions to endentulism by osteoporosis and cigarette smoking. Arch Intern Med. 1983;143(9):1678-82.
- Krall EA, Dawson-Hughes B, Papas A, Garcia RI. Tooth loss and skeletal bone density in healthy postmenopausal women. Osteoporos Int. 1994;4(2):104-9.
- Krall EA, Garcia RI, Dawson-Hughes B. Increased risk of tooth loss is related to bone loss at the whole body, hip, and spine. Calcif Tissue Int. 1996;59(6):433-7.
- Hildebolt CF, Pilgram TK, Dotson M, Yokoyama-Crothers N, Muckerman J, Hauser J, et al. Attachment loss with postmenopausal age and smoking. J Periodontal Res. 1997;32(7):619-25.
- Bando K, Nitta H, Matsubara M, Ishikawa I. Bone mineral density in periodontally healthy and edentulous postmenopausal women. Ann Periodontol. 1998;3(1):322-6.
- Yoshihara A, Seida Y, Hanada N, Nakashima K, Miyazaki H. The relationship between bone mineral density and the number of remaining teeth in community-dwelling older adults. J Oral Rehabil. 2005;32(10):735-40.
- Famili P, Cauley J, Suzuki JB, Weyant R. Longitudinal study of periodontal disease and endentulism with rates of bone loss in older women. J Periodont. 2005;76(1):11-5.
- Earnshaw SA, Keating N, Hosking DJ, Chilvers CE, Ravn P, McClung M, Wasnich RD. Tooth counts do not predict bone mineral density in early postmenopausal Caucasian women. Int J Epidemiol. 1998;27(3):497-83.
- Eastell R. Role of oestrogen in the regulation of bone turnover at the menarche. J Endocrinol. 2005;185(2):223-34.
- Gibson RS. Principals of nutritional assessment. 2nd ed. Oxford, Oxford University Press; 2005.
- Statistics Canada. Eating well with Canada's Food Guide. Ottawa, ON: Health Canada; 2011. Available: www.hc-sc.gc.ca/fn-an/food-guide-aliment/index-eng.php (accessed 2012 Feb 16).
- Papaioannou A, Morin S, Cheung AM, Atkinson S, Brown JP, Feldman S, et al. Scientific Advisory Council of Osteoporosis Canada. 2010 clinical practice guidelines for the diagnosis and management of osteoporosis in Canada: summary. CMAJ. 2010;182(17):1864-73. Epub 2010 Oct 12.
- Hanley DA, Cranney A, Jones G, Whiting SJ, Leslie W; Guidelines Committee of the Scientific Advisory Council of Osteoporosis Canada. Vitamin D in adult health and disease: a review and guideline statement from Osteoporosis Canada (summary). CMAJ. 2010;182(12):1315-9. Epub 2010 Jul 12.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911-30. Epub 2011 Jun 6.