A 54-year-old woman was referred to our department for evaluation of painful gum swelling in the lower anterior region of 3 months' duration. The patient reported sudden onset of the swelling, which covered almost half of the lower anterior teeth. The swollen tissue was bright red and was associated with severe pain, which interfered with speech, mastication and sleep. Over the month following onset of the gingival swelling, she had experienced sudden, painful bilateral swelling of the neck, restriction of mouth opening and ear blockage. The patient had known hypertension and had been taking atenolol 25 mg once daily for the past 2 years. She reported no tobacco-related oral habits.
Extraoral examination revealed bilateral enlargement of the submandibular salivary glands (Fig. 1) and severe restriction of mouth opening (< 2 cm). The swollen tissue was mildly tender on palpation, had a firm consistency and was fixed. Examination of the temporomandibular joint revealed no obvious abnormalities. Intraoral examination showed that the enlargement affected the marginal, interdental and attached gingiva in the lower anterior region, extending from tooth 45 to tooth 35. The bright red surface appeared granular, with numerous short bulbous projections, simulating the appearance of an overripe strawberry (Fig. 2). The gingiva was soft and friable, and there was minimal bleeding on manipulation. The lingual gingiva and edentulous areas were unaffected. The upper interdental gingiva in the facial aspect also showed mild granular hyperplasia.
Intraoral, extraoral and chest radiographs did not reveal any abnormalities, but the erythrocyte sedimentation rate was elevated (125 mm/h; normal range 0–20 mm/h), as was the total white blood cell count (16 × 109/L; normal range 4 × 109/L to 10 × 109/L). Aspartate aminotransferase and alanine aminotransferase were mildly elevated, but the results of renal function tests and urinalysis were within normal ranges. Histopathologic examination of gingival tissue obtained by biopsy showed that the epithelium was hemorrhagic, with multiple intraepithelial microabscesses; however, these findings were inconclusive. Cutaneous vasculitis of both legs developed within 2 weeks of presentation (Fig. 3).
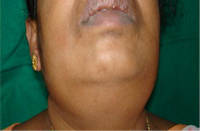 Figure 1: Extraoral photograph showing bilateral enlargement of the submandibular salivary glands.
Figure 1: Extraoral photograph showing bilateral enlargement of the submandibular salivary glands.
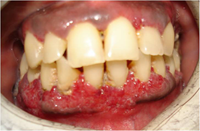 Figure 2: Intraoral clinical photograph showing enlargement of the lower anterior gingiva. The swollen tissue is characterized by its granularity, short bulbous projections and bright red colour. The appearance resembles that of an overripe strawberry.
Figure 2: Intraoral clinical photograph showing enlargement of the lower anterior gingiva. The swollen tissue is characterized by its granularity, short bulbous projections and bright red colour. The appearance resembles that of an overripe strawberry.
 Figure 3: Cutaneous vasculitis developed during the course of the patient's illness.
Figure 3: Cutaneous vasculitis developed during the course of the patient's illness.
What is this condition?
Differential Diagnosis
For patients presenting with the symptoms described above, a number of conditions must be considered in the differential diagnosis.
Drug-Induced Gingival Enlargement
Phenytoin, cyclosporine A, calcium-channel blockers and oral contraceptives are the agents that most commonly cause drug-induced gingival enlargement.1,2 This problem usually manifests as painless, beadlike (smooth), firm enlargement of the gingiva, with no change in colour. The swelling typically starts in the interdental gingiva and progresses to involve the marginal and attached gingivae. The enlargement is usually generalized throughout the mouth but is more severe in the maxillary and mandibular anterior region. Pain occurs only if there is secondary bacterial or fungal infection.
Leukemic Gingival Infiltration
Both the acute and chronic forms of all types of leukemia may have oral manifestations, but these features are more frequently seen in the acute phase.3 The oral complications of leukemia frequently include gingival hypertrophy, petechiae, ecchymosis, mucosal ulcers and hemorrhage.3 Leukemic infiltration into the gingival tissues can lead to generalized gingival enlargement. The enlarged tissues are usually soft, shiny, erythematous and highly tender, and they bleed on palpation. The diagnosis of leukemia is made by identifying blast cells in the peripheral blood and bone marrow.4
Lymphoma
The lymphomas are a group of malignant solid tumours involving cells of the lymphoreticular system. The most common presentation is painless, persistent enlargement of the lymph nodes, but extranodal lesions may also occur, especially in cases of non-Hodgkin lymphoma.4 Oral non-Hodgkin lymphoma often mimics inflammatory disease and may present as a gingival mass, a tongue mass or an intraosseous lesion. A gingival lesion may appear as a gingival enlargement with a smooth or ulcerated surface and may be the first manifestation of the disease.3 Radiographic, hematologic and histopathologic evaluation is required to establish the diagnosis.
Primary or Metastatic Carcinoma of Gingiva
Primary and metastatic carcinomas arising from the gingival tissue may be erythematous, ulcerative, granular or proliferative in nature. The similarity between early cancerous lesions of the gingiva and dental infection has frequently led to a delay in diagnosis.5 Metastasis to the jaw from breast, lung, kidney and other regions is common, but metastasis to the oral soft tissues is extremely rare (0.1%) and frequently involves the gingiva.5 The mandibular gingiva, especially the attached gingiva, is more frequently affected. Histopathology plays a key role in making the definitive diagnosis.5
Wegener Granulomatosis
Wegener granulomatosis is a rare multisystem disorder characterized by a classic triad of necrotizing granulomatous inflammation of the upper and lower respiratory tracts, glomerulonephritis and systemic vasculitis. In the early stages of the disease, the most common presentation is sinusitis (exhibited by 73% of patients), followed by lung problems, including cough, hemoptysis or radiographic evidence of infiltrates or cavitations.6 It may affect almost any organ of the body, including the eyes, ears, brain, skin, joints, heart and sexual organs. Oral manifestations, seen in only 6% to 13% of cases, are rare and may be in the form of nonspecific oral ulcerations (relatively common) or strawberry gingivitis (extremely rare, occurring in just 2% of cases).6 Delay of healing of extraction sockets occurs as a complication of the later stages of disease, particularly if renal failure develops. Unilateral or bilateral enlargement of the salivary glands is seen infrequently. Antineutrophil cytoplasmic antibody (ANCA) testing is now suggested as a rapid and noninvasive way to diagnose Wegener granulomatosis,7,8 because a positive cytoplasmic pattern of ANCA staining (c-ANCA) is strongly associated with this disease.
Microscopic Polyangiitis
Microscopic polyangiitis is characterized by small-vessel vasculitis, which rapidly progresses to glomerulonephritis, lung vasculitis, arthritis and myalgia. As such, this condition simulates Wegener granulomatosis at a clinical level. It is diagnosed by means of histopathologic evaluation, which reveals nongranulomatous pulmonary and renal necrotizing vasculitis (in contrast to the granulomatous vasculitis seen in Wegener granulomatosis). ANCA levels are also raised in microscopic polyangiitis, but in this disease the perinuclear pattern of staining (p-ANCA) is frequently raised to a greater extent than c-ANCA.9
Orofacial Granulomatosis
Orofacial granulomatosis is a term used to describe the occurrence of granulomas in the orofacial region in the absence of any recognized systemic condition. Typically, orofacial granulomatosis presents as recurrent, persistent labial swellings, which result in enlargement of the lips. This condition may also be associated with oral ulceration, painless gingival overgrowth and a cobblestone appearance of the buccal mucosa. Histopathologic examination reveals noncaseating epithelioid cell granulomas and lymphedema. These histologic features are indistinguishable from those of Crohn disease and sarcoidosis.10 However, clinical correlation helps in differentiating these conditions.
Sarcoidosis
Sarcoidosis is a multiorgan disorder of unknown etiology which usually presents with pulmonary infiltration and hilar lymphadenopathy. Involvement of the eyes, skin and salivary glands is relatively common. Sarcoidosis rarely involves the oral cavity, although it has been reported to affect the buccal mucosa, tongue, lips, palate, floor of the mouth, mandible and maxilla.3,10,11 Gingival involvement in sarcoidosis causes enlargement with occasional ulceration, identical to orofacial granulomatosis. This feature may be the first clinical sign of the disease. Histologically, sarcoidosis presents as a noncaseating granuloma, accompanied by epithelioid histiocytes rimmed with lymphocytes and scattered Langhans or foreign body-type giant cells.
Crohn Disease
Crohn disease is a chronic granulomatous disorder of unknown etiology that affects mainly the ileum but may affect any part of the gastrointestinal tract, including the mouth. Oral manifestations include multiple intraoral ulcerations similar to those of aphthous stomatitis, a cobblestone appearance of the buccal mucosa, diffuse firm enlargement of the lips and reddish granulomatous enlargement of the gingiva. Orofacial manifestations are identical with those of orofacial granulomatosis, but they are usually associated with active intestinal disease.10,11
Bacterial and Deep Fungal Infections
Infective conditions that can cause granulomatous inflammation, such as tuberculosis12 and deep fungal infections,3 should also be considered in a case such as the one described here. Lesions may occur on the gingiva, tongue, vestibule and buccal mucosa. They appear as diffuse, hyperemic, nodular or papillary proliferations or ulcers. Bacterial infections, particularly in immunocompromised patients, may produce erythematous, hyperplastic and necrotizing gingivitis. The definitive diagnosis should be reached by histopathologic examination, along with the use of specific stains to identify the causative organism.
Diagnosis of the Patient
In the case presented here, the histopathologic examination did not reveal any granulomatous changes, which allowed us to rule out conditions such as orofacial granulomatosis, sarcoidosis and Crohn disease. The hemogram and histopathology did not conclusively point to any neoplastic processes. The drug history did not indicate any agent known to cause drug-induced gingival enlargement. The characteristic strawberry appearance of the gingiva suggested Wegener granulomatosis. However, bilateral enlargement of the salivary glands, as seen in this case, is an exceedingly rare manifestation of this condition. ANCA serological testing was advised, and the result was strongly positive for c-ANCA antibodies. Wegener granulomatosis was diagnosed, and treatment was instituted promptly.
Discussion
Wegener granulomatosis is considered a great masquerader, because it may present with a wide range of clinical appearances, most of which are nonspecific. This may lead to a delay in diagnosis or even misdiagnosis. Detailed laboratory investigations, including complete hemogram, measurement of C-reactive protein and renal function tests, should be performed to determine the extent of multiorgan involvement. The c-ANCA value is considered to be a sensitive and specific marker for multisystem Wegener granulomatosis (specificity 95% to 100%, sensitivity 22% to 100%)7 and may be helpful in tracking disease activity and possible relapse. Histopathologic criteria for the diagnosis of Wegener granulomatosis require identification of vasculitis, ill-defined granulomas, multinucleated giant cells and necrosis. However, these features are usually evident only in biopsy samples of the lung and are usually absent from most biopsy specimens of oral lesions.6 The patient described here also presented with cutaneous vasculitis in both legs, which was an additional contributory finding relevant to the final diagnosis. However, vasculitis is not pathognomonic for Wegener granulomatosis, and it may be present in a wide array of diseases, such as temporal arteritis, polyarteritis nodosa, Kawasaki disease, Churg–Strauss syndrome, microscopic polyangiitis, Henoch–Schönlein purpura, cryoglobulinemic vasculitis and cutaneous leukocytoclastic angiitis.7 Hence, the recognition of oral symptoms plays a pivotal role in narrowing the differential diagnosis of vasculitis.
Management of Wegener granulomatosis requires a multidisciplinary approach and depends on the stage at which diagnosis is made. The mainstay of treatment is combined therapy with corticosteroids and immunosuppressants (mainly cyclophosphamide 2 mg/kg daily).6,13 Initial high-dose glucocorticoid therapy (prednisolone 1 mg/kg daily) is followed by maintenance therapy (tapered doses of prednisolone).6,13,14 About 90% of patients undergoing this form of therapy experienced significant improvement, and 75% had complete remission,14,15 but side effects of the drugs are inevitable. Other suggested treatment modalities include the use of trimethoprim–sulfamethoxazole as an adjuvant to reduce rates of relapse and other complications.16 Intravenous immunoglobulin and plasmapheresis are used in refractory cases.17 Our patient showed dramatic response to dexamethasone by injection 8 mg every 8 hours for 10 days. Within a week, almost 90% of the gingival lesions had resolved, and most of the enlargement of the submandibular salivary glands had subsided. This treatment was followed by prednisolone 50 mg/day (administered orally), which was gradually tapered to a low maintenance dose. Because the patient had cutaneous vasculitis, cyclophosphamide 100 mg/day was started as adjuvant therapy, and there was dramatic improvement within 2 weeks. At the time of writing, the patient had been receiving regular follow-up for 3 years and was asymptomatic.
Early diagnosis of this life-threatening disease is crucial, as the diagnosis plays an important role in treatment and prognosis. As the disease progresses, the majority of patients experience renal disease, with renal failure being the most common cause of death. In 82% of cases that go undiagnosed or untreated, the patient will not survive more than a year.15,18 However, with early initiation of appropriate treatment, up to 75% of patients with Wegener granulomatosis can expect significant or even complete remission.15
For several reasons, identification of strawberry gingiva is important in early diagnosis and treatment, and its presence is therefore associated with a better prognosis.7,18,19 This unusual presentation of the gingiva, simulating an overripe strawberry, is often the earliest manifestation of Wegener granulomatosis. The swelling remains localized in the oral cavity for days to months before it progresses to fatal pulmonary and renal involvement. The appearance of strawberry gingiva is unique, distinct and pathognomonic, which makes it readily identifiable by an expert dental practitioner. Once the diagnosis has been made, medical treatment can be instituted promptly, which will dramatically improve the prognosis for patients with this serious, potentially fatal disorder.
THE AUTHORS
References
- Trackman PC, Kantarci A. Connective tissue metabolism and gingival overgrowth. Crit Rev Oral Biol Med. 2004:15(3):165-75. Review
- Abdollahi M, Radfar M,. A review of drug-induced oral reactions. J Contemp Dent Pract. 2003;4(1):10-31. Review.
- Stewart C, Cohen D, Bhattacharyya I, Scheitler L, Riley S, Calamia K, et al. Oral manifestations of Wegener's granulomatosis: a report of three cases and a literature review. J Am Dent Assoc. 2007;138(3):338-48.
- DeRossi SS, Garfunkel A, Greenberg MS. Hematologic diseases. In: Greenberg MS, Glick M, editors. Burket's oral medicine: diagnosis and treatment. 10th ed. Hamilton, Canada: BC Decker Inc; 2003. p. 429-453.
- Epstein J. Oral cancer. In: Greenberg MS, Glick M, editors. Burket's oral medicine. 10th ed. Canada: Hamilton, Canada: BC Decker Inc; 2003. p.195-234.
- Ponniah I, Shaheen A, Shanker KA, Kumaran MG. Wegener's granulomatosis: the current understanding. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100(3):265-70.
- Abdul-Aziz K, Faizal AA. Immunological diagnosis of vasculitis. Saudi Med J. 2006;27(8):1105-15.
- Rao JK, Weinberger M, Oddone EZ, Allen NB, Landsman P, Feussner JR. The role of antineutrophil cytoplasmic antibody (c-ANCA) testing in the diagnosis of Wegener's granulomatosis. A literature review and meta-analysis. Ann Intern Med. 1995;123(2):925-32.
- Shiboski CH, Regezi JA, Sanchez HC, Silverman S Jr. Oral lesions as the first clinical sign of microscopic polyangiitis: a case report. Oral Surg Oral Pathol Oral Radiol Endod. 2002;94(6):707-11.
- Grave B, McCullough M, Wiesenfeld D. Orofacial granulomatosis—a 20-year review. Oral Dis. 2009;15(1):46-51.
- Batal H, Chou LL, Cottrell DA. Sarcoidosis: medical and dental implications. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(8):386-90.
- Karthikeyan BV, Pradeep AR, Sharma CG. Primary tuberculous gingival enlargement: a rare entity. J Can Dent Assoc. 2006;72(7):645-8.
- Fauci AS, Haynes BF, Katz P, Wolff SM. Wegener's granulomatosis: prospective clinical and therapeutic experience with 85 patients for 21 years. Ann Intern Med. 1983(1);98:76-85.
- Hoffman GS, Kerr GS, Leavitt RY, Hallahan CW, Lebovics RS, Travis WD, et al. Wegener granulomatosis: an analysis of 158 patients. Ann Intern Med. 1992;116(6):488-98.
- Clark WJ, Broumand V, Rustin JD, Davenport WL. Erythematosus, granular, soft tissue lesion of the gingiva. J Oral Maxillofac Surg. 1998;56(8):962-7.
- Stegeman CA, Tervaert JW, De Jong PE, Kallenberg CG. Trimethoprim-sulfamethoxazole(co-trimoxazole) for the prevention of relapses of Wegener's granulomatosis. Dutch Co-Trimoxazole Wegener Study Group. N Engl J Med. 1996;335(1):16-20.
- Jayne DR, Gaskin G, Rasmussen N, Abramowicz D, Ferrario F, Guillevin L, et al. Randomized trial of plasma exchange or high-dosage methylprednisolone as adjunctive therapy for severe renal vasculitis. J Am Soc Nephrol. 2007;18(7):2180-8. Epub 2007 Jun 20.
- Lilly J, Juhlin T, Lew D, Vincent S, Lilly G. Wegener's granulomatosis presenting as oral lesions: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;85(2):153-7.
- Eufinger H, Machtens E, Akuamoa-Boateng E. Oral manifestations of Wegener's granulomatosis. Review of literature and report of a case. Int J Oral Maxillofac Surg. 1992;21(1):50-3.
