Abstract
Objective: To describe the prevalence of oral pain in Canada and to identify its covariates.
Methods: Data were derived from the 2007-2009 Canadian Health Measures Survey. Data were analyzed for a total of 5284 respondents (2558 males, 2726 females) aged 6-79 years. The outcome variable was self-reported pain in the mouth in the past 12 months. Bivariate and multivariate analyses were used to investigate the relationship between oral pain and 4 sets of covariates: socio-demographic factors, dental service utilization, oral health behaviours and clinical oral health.
Results: Oral pain in the past 12 months was reported by 11.7% of respondents. Oral pain was slightly, but not significantly, more prevalent among females than males (13.6% vs. 10.0%). The lowest and highest prevalence of oral pain were reported by children and young adults, respectively. Multivariate analyses suggested that oral pain was significantly more prevalent among adolescents and adults, those in the lowest income groups, those who avoided a dental professional because of the cost and those with untreated decayed teeth.
Conclusion: Canadians with financial barriers to accessing dental care and those with untreated dental decay were at risk of having dental pain. These findings have important implications for the provision of dental care in Canada.
Oral pain is a common symptom of oral health conditions. It affects an individual’s daily life activities, such as eating, sleeping and social functioning,1-5 and adversely affects society, through absenteeism (i.e., time lost from work or school).1,6,7 Oral pain is also a major factor in seeking dental treatment.8,9
Obtaining information about oral pain has become an important component of national health surveys. The prevalence of toothache in the past 6 months was 14.5% among US adults in the 1989 National Health Interview Survey,10 and painful aching in the past 12 months was reported by 28% of participants in the 1998 UK Adult Oral Health Survey.11 There have been some reports on oral pain among Canadians,5,7 but those studies were limited, in that they reported data for samples that were not nationally representative or they did not examine the covariates of oral pain.
The 2007-2009 Canadian Health Measures Survey (CHMS) has set the scene for informing policy-makers about the prevalence of oral pain and its covariates. This study was undertaken to describe the prevalence of oral pain in Canada and to identify its covariates.
Methods
Data Source
Data for this study were obtained from the 2007–2009 CHMS, the most recent national health survey of the Canadian population collecting data on oral health indicators. The CHMS is a probabilistic, multistage, stratified survey of households. The sampling framework ensures representativeness of the Canadian population, by the collection of data from different age–sex groups sampled from several sites across Canada, stratified by region. The CHMS aimed to provide national estimates by collecting data from several sites covering 97% of the population of Canada. The 2007-2009 CHMS collected data from 5604 Canadians aged 6-79 years. For the current analysis, adults with no teeth in the upper and lower jaws (n = 302) were excluded. In addition, 18 respondents who did not attend dental examination were excluded from analyses. The methodology and sampling framework of the CHMS have been described by Statistics Canada.12
Oral Pain
The experience of oral pain was determined through the following question: “In the past 12 months, how often have you had any other persistent or ongoing pain anywhere in your mouth?” Participants reported the frequency of pain by selecting one of the following answers: never, rarely, sometimes or often. For the purpose of data analysis, the frequency of dental pain was dichotomized as persistent pain (sometimes or often) and no persistent pain (never or rarely). This classification was also adopted by the technical report on the oral health findings of the CHMS published by Health Canada.13
Covariates
Four sets of covariates were included in the analyses: socio-demographic factors, dental service utilization, oral health behaviours and clinical oral health. The socio-demographic factors were sex, age-group, racial background, country of birth, equivalized household income, education and ownership of the dwelling by a member of the household. Equivalized household income was calculated using the OECD (Organisation for Economic Co-operation and Development) modified equivalence scale, which takes into account the number and ages of people in each household.14 Education reflected the highest level of education achieved by any member of the household. Indicators of dental service utilization consisted of visiting a dental professional in the past 12 months, avoiding seeing a dental professional in the past 12 months because of the cost, having dental insurance and pattern of dental visit (check-up or treatment vs. emergency care only). Indicators of oral health behaviours were tooth-brushing and dental flossing. Indicators of clinical oral health were presence of untreated decayed teeth and overall periodontal health. The CHMS Dentist's Survey Manual and Coding Criteria (available upon request to the corresponding author) described the procedure for examining decayed teeth. A tooth was considered decayed if there was any smooth-surface caries in the crown. In terms of periodontal health, participants were classified as healthy or unhealthy, according to the extent of clinical attachment loss: those with attachment loss of 4 mm or more were considered to have an unhealthy periodontal condition, and those with attachment loss of less than 4 mm were considered to have a healthy periodontal condition. This classification was also employed by the technical report on the oral health findings of the CHMS.13
Data Analysis
Bivariate and multivariate analyses were performed, taking into account sample weights to provide estimates representative of the Canadian population. STATA 11.1 software (StataCorp LP, College Station, TX) was used for the analyses. A multivariate logistic regression model was constructed to identify the independent relationship of covariates with oral pain. Only variables with p value less than 0.25 for at least one category in the bivariate analyses were entered into the multivariate model. The 4 groups of variables associated with oral pain—socio-demographic factors, indicators of dental service utilization, oral health behaviours and clinical oral health outcomes—were entered into the model sequentially. The significance level for the multivariate model was set at p < 0.05. Interactions of sex and age with income, avoidance of dental professionals because of cost and presence of untreated decayed teeth were tested. None of these interactions were significant, so sex- and age-stratified multivariate models were not constructed.
Results
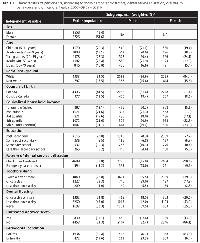
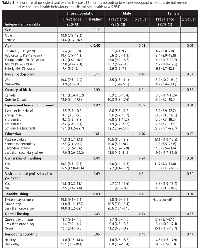
Data were analyzed for 5284 individuals (2558 males and 2726 females). Most respondents were white (84.5%), most had post-secondary education (78.0%), and most had visited a dental professional in the past 12 months (80.3%) (Table 1). Oral pain was reported by 11.7% of the study population. Oral pain was slightly more prevalent among females than males, but the difference was not statistically significant (13.6% vs. 10.0%; p = 0.13). Three socio-demographic factors were significantly related to oral pain at the bivariate analytic level: age (p < 0.001), income (p = 0.02) and ownership of dwelling (p = 0.01) (Table 2). The prevalence of oral pain was lowest and highest among children and young adults, respectively (Table 2, Fig. 1), and this pattern was present for both sexes. Oral pain was more prevalent among individuals who avoided a dental professional because of the cost (p < 0.001) and those who never visited a dental professional or did so only for emergency care (p = 0.01). Individuals who reported brushing their teeth more frequently were less likely to report oral pain (p = 0.03). Oral pain was significantly related to the presence of untreated decayed teeth (p < 0.001) but not to unhealthy periodontal condition (p = 0.96). Stratified bivariate analyses of the data for the male and female population suggested that covariates of oral pain varied according to sex (Table 2). All variables that were significantly related to oral pain for the total population were also significantly related to oral pain for female participants. However, only 3 of these variables (age, avoiding a dental professional because of cost and presence of untreated decayed teeth) were significant in the analysis of male participants.
 Figure 1: Sex-stratified distribution of oral pain by age group. The prevalence of oral pain varied significantly by age (p < 0.001) but not by sex (p = 0.13).
Figure 1: Sex-stratified distribution of oral pain by age group. The prevalence of oral pain varied significantly by age (p < 0.001) but not by sex (p = 0.13).
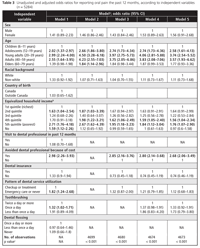
In the final model, age, income, avoiding a dental professional because of cost and presence of untreated decayed teeth were significant covariates of oral pain (model 5 in Table 3). Adolescents, young adults and adults were at significantly higher risk of oral pain than children. The prevalence of oral pain was significantly higher among those in the 2 lowest income quintiles than among those in the highest income quintile. Those who avoided a dental professional because of cost were 2.68 times (95% confidence interval 2.06–3.49) more likely to report oral pain. The odds of reporting oral pain were 1.58 times greater (95% confidence interval 1.07–2.32) among those with untreated decayed teeth than among those without such teeth.
Discussion
This paper reports the prevalence of oral pain and its covariates on the basis of data from the 2007-2009 CHMS. Oral pain affects a large number of Canadians. Specifically, more than one-tenth of survey respondents reported oral pain in the past 12 months. Because of methodologic differences, such as variation in the recall period for which participants reported oral pain, it was difficult to compare the results of this analysis with those of other studies. In a 2008 national telephone interview survey of Canadians, only 5% of participants reported “painful aching in the mouth” within the previous month.7 In contrast, a 1985 mail survey of people living in Toronto reported a 14.1% prevalence of “toothache” in the past 4 weeks among adults.15
The current study found that oral pain in Canada was more prevalent among adolescents and adults (than among children), lower income groups, those who avoided a dental professional because of the cost and those with untreated decayed teeth.
There was no difference in reporting of oral pain between males and females. This finding is consistent with some studies of oral pain,5,10,15-17 although others have reported higher prevalence of oral pain among males18 or females.11,19-21 When the data were analyzed by age-group, children had the lowest prevalence of oral pain. In the CHMS, parents or guardians answered questions about their children aged 6 to 11 years, which might have affected the findings. Nevertheless, it has been shown that parents can provide accurate information about their children’s oral health status.22 Among adults, there was an inverse relationship between age and oral pain, in agreement with the literature.10,11,19 The decrease in oral pain among elderly people can be attributed to a decline in the number of natural teeth and, accordingly, a reduction in the number of decayed teeth.19 An alternative explanation is the lower expectations for oral health among older age groups, which leads to better results for self-reported outcomes such as oral pain.23
The finding that oral pain was more prevalent among lower income groups confirms previous findings reported in the literature.10,11,16,19,20,24-26 Interestingly, the relationship between income and oral pain remained significant after controlling for indicators of dental service utilization and clinical oral health (see model 5 in Table 3), suggesting that these variables are unlikely to provide the full explanation for this relationship. It is possible that factors other than those investigated in this study transfer the effect of socio-economic status to oral pain.
In the final model, avoiding dental visits because of the cost was related to reporting more oral pain, whereas dental insurance was not a significant covariate. In other words, having dental insurance did not fully address financial barriers to oral health care. It is possible that those suffering from oral pain face other barriers to oral health care, even if they have dental insurance.27 The provision of dental insurance varies from one person to another in terms of treatments that are covered and levels of reimbursement, which may have influenced this finding. In addition, visiting a dental professional in the past 12 months and visiting dental professionals for check-ups or treatment were not associated with reporting oral pain. The possibility of treatment-induced pain, the quality of treatment, fear of dental treatment and severity of pain are among the factors that might influence the relationship between oral pain and visiting a dental professional. Nonetheless, in contrast with the current findings, previous studies have reported that dental pain was less prevalent among those who visited a dentist in the past year,28 those who visited a dentist for check-ups16 and those with dental insurance coverage.10
Consistent with previous findings,1,10,16 having untreated decayed teeth increased the odds of reporting oral pain. The severity of decay also increases the risk of dental pain.16
Tooth-brushing and dental flossing were not related to oral pain in this study. Other evidence is contradictory with regard to the relationship between oral health behaviours and pain, with some studies having found no relationship28 and others having found that pain was less prevalent among those who brushed more frequently.17,20 The latter finding may be related to the observation from this study that untreated decay is related to pain: given that the majority of people use fluoride toothpaste, those who clean their teeth more often are likely to have less decay and therefore less pain. However, the relationships between oral hygiene and periodontal disease and between periodontal disease and pain in general are much more ambiguous, so it is not surprising that this study found no relationship between flossing and pain.
In this study, there was no relationship between pain and racial background, although this factor was an established determinant of major oral health outcomes, including oral pain, in one study of US adults.10 The particular historical context in the United States has led to regular use of this indicator for this type of study, but its relevance in Canada is questionable. Nevertheless, data on racial background were collected in the CHMS survey, and this variable was used here as the only indicator of ethnic background available for analysis. Given its questionable validity in the Canadian context, it is unsurprising that racial background was not associated with oral pain.
The terminology used in the literature on oral pain has been inconsistent. In particular, it is important to distinguish between oral pain, which is felt in the mouth, and orofacial pain, which encompasses pain in the neck and head. Furthermore, some studies have employed other terms, such as “dental pain,” “toothache” or “tooth pain” to refer to pain in the mouth. Although pain in the mouth can originate from tooth-related problems, oral pain may not be precisely represented by the terms “dental pain,” “toothache” or “tooth pain.” More specifically, the term “oral pain” indicates any pain within the mouth, whereas dental pain has been described as “pain that originates from innervated tissues within the tooth or immediately adjacent to it.”29
Some of the important limitations of this study were its cross-sectional design, which precludes causal inference between covariates and oral pain, and inherent recall bias for questions concerning previous experience of oral pain and oral health-related behaviours. There is also the possibility of response bias (e.g., some individuals over-reporting their oral health behaviours). Several other factors, such as smoking, are potentially related to oral pain19,21,28 but were not investigated in this study. The CHMS did not gather data on smoking among children, so inclusion of smoking as a covariate in the analyses for all age groups would have resulted in many missing data. In future studies, researchers may wish to analyze the CHMS data for adults separately, not only to investigate the effect of smoking but also because some of the covariates that were investigated (e.g., periodontal disease) might be more prevalent in older populations.
This study has important implications for oral health policy in Canada. We suggest that oral health policies in this country direct resources toward pain-relieving treatment for adolescents and adults, among whom the prevalence of oral pain was higher than among children and elderly people. The higher prevalence of oral pain in lower-income groups might ideally be dealt with from the perspective of social determinants of health, through redistribution of income, but this may not be achievable through health policy alone. However, lower-income groups should receive assistance in accessing treatment, at least in terms of pain relief, which would have immediate effects on oral health conditions and quality of life. Financial barriers to oral health care represented an important covariate of oral pain, which should be tackled by protecting those who face such barriers or by providing dental treatments to as large a proportion of the Canadian population as possible. Oral health policies should also focus on tackling untreated oral disease. If reducing levels of oral pain in the Canadian population is adopted as a goal of oral health care policy, then our findings indicate that targeting untreated dental decay is likely to have an effect, whereas managing periodontal disease is unlikely to reduce oral pain.
THE AUTHORS
References
- Ratnayake N, Ekanayake L. Prevalence and impact of oral pain in 8-year-old children in Sri Lanka. Int J Paediatr Dent. 2005;15(2):105-12.
- Mashoto KO, Astrom AN, David J, Masalu JR. Dental pain, oral impacts and perceived need for dental treatment in Tanzanian school students: a cross-sectional study. Health Qual Life Outcomes. 2009;7:9.
- Goes PS, Watt RG, Hardy R, Sheiham A. Impacts of dental pain on daily activities of adolescents aged 14-15 years and their families. Acta Odontol Scand. 2008;66(1):7-12.
- Cohen LA, Bonito AJ, Eicheldinger C, Manski RJ, Macek MD, Edwards RR, et al. Behavioral and socioeconomic correlates of dental problem experience and patterns of health care-seeking. J Am Dent Assoc. 2011;142(2):137-49.
- Locker D, Grushka M. The impact of dental and facial pain. J Dent Res. 1987;66(9):1414-7.
- Shepherd MA, Nadanovsky P, Sheiham A. The prevalence and impact of dental pain in 8-year-old school children in Harrow, England. Br Dent J. 1999;187(1):38-41.
- Quinonez C, Figueiredo R, Locker D. Disability days in Canada associated with dental problems: a pilot study. Int J Dent Hyg. 2011;9(2):132-5.
- Duncan RP, Gilbert GH, Peek CW, Heft MW. The dynamics of toothache pain and dental services utilization: 24-month incidence. J Public Health Dent. 2003;63(4):227-34.
- Al-Omiri MK, Al-Wahadni AM, Saeed KN. Oral health attitudes, knowledge, and behavior among school children in North Jordan. J Dent Educ. 2006;70(2):179-87.
- Vargas CM, Macek MD, Marcus SE. Sociodemographic correlates of tooth pain among adults: United States, 1989. Pain. 2000;85(1-2):87-92.
- Pau A, Croucher RE, Marcenes W. Demographic and socio-economic correlates of dental pain among adults in the United Kingdom, 1998. Br Dent J. 2007;202(9):E21; discussion 548-9. Epub 2007 Feb 23.
- Statistics Canada. Canadian Health Measures Survey (CHMS). Accessed 2012 Feb. Available: http://www.statcan.gc.ca/imdb-bmdi/5071-eng.htm.
- Health Canada. Report on the Findings of the Oral Health Component of the Canadian Health Measures Survey 2007- 2009. Accessed 2012 Feb. Available: http://www.hc-sc.gc.ca/ahc-asc/branch-dirgen/fnihb-dgspni/ocdo-bdc/project-eng.php.
- Organisation for Economic Co-operation and Development (OECD). What Are Equivalence Scales? Accessed 2012 Feb. Available: http://www.oecd.org/dataoecd/61/52/35411111.pdf
- Locker D, Grushka M. Prevalence of oral and facial pain and discomfort: preliminary results of a mail survey. Community Dent Oral Epidemiol. 1987;15(3):169-72.
- Goes PS, Watt R, Hardy RG, Sheiham A. The prevalence and severity of dental pain in 14-15 year old Brazilian schoolchildren. Community Dent Health. 2007;24(4):217-24.
- Honkala E, Honkala S, Rimpela A, Rimpela M. The trend and risk factors of perceived toothache among Finnish adolescents from 1977 to 1997. J Dent Res. 2001;80(9):1823-7.
- Bassols A, Bosch F, Campillo M, Canellas M, Banos JE. An epidemiological comparison of pain complaints in the general population of Catalonia (Spain). Pain. 1999;83(1):9-16.
- Bastos JL, Gigante DP, Peres KG. Toothache prevalence and associated factors: a population based study in southern Brazil. Oral Dis. 2008;14(4):320-6.
- Jung SH, Watt RG, Sheiham A, Ryu JI, Tsakos G. Exploring pathways for socio-economic inequalities in self-reported oral symptoms among Korean adolescents. Community Dent Oral Epidemiol. 2011;39(3):221-9.
- Lahti S, Sipila K, Taanila A, Laitinen J. Oral pain and associated factors among adolescents in northern Finland. Int J Circumpolar Health. 2008;67(2-3):245-53.
- Piovesan C, Marquezan M, Kramer PF, Bonecker M, Ardenghi TM. Socioeconomic and clinical factors associated with caregivers’ perceptions of children’s oral health in Brazil. Community Dent Oral Epidemiol. 2011;39(3):260-7. Epub 2010 Dec 29.
- Atchison KA, Gift HC. Perceived oral health in a diverse sample. Adv Dent Res. 1997;11(2):272-80.
- Peres MA, Peres KG, Frias AC, Antunes JL. Contextual and individual assessment of dental pain period prevalence in adolescents: a multilevel approach. BMC Oral Health. 2010;10:20.
- Lewis C, Stout J. Toothache in US children. Arch Pediatr Adolesc Med. 2010;164(11):1059-63.
- Riley JL 3rd, Gilbert GH, Heft MW. Socioeconomic and demographic disparities in symptoms of orofacial pain. J Public Health Dent. 2003;63(3):166-73.
- Schrimshaw EW, Siegel K, Wolfson NH, Mitchell DA, Kunzel C. Insurance-related barriers to accessing dental care among African American adults with oral health symptoms in Harlem, New York City. Am J Public Health. 2011;101(8):1420-8. Epub 2011 Jun 16.
- Unell L, Söderfeldt B, Halling A, Birkhed D. Explanatory models for clinically determined and symptom-reported caries indicators in an adult population. Acta Odontol Scan. 1999;57(3):132-38.
- Sharav Y. Orofacial pain. In: Wall PD, Melzack R, editors. Textbook of pain. Edinburgh: Churchill Livingstone; 1994.