Postoperative Pain Following Periodontal Surgery
Pain may occur following a periodontal surgery that involves the opening of a flap, gingival grafts, or gingivectomy/frenectomy procedures. Postoperative pain experienced within the first 3 days after surgery is considered normal and should progressively diminish throughout the healing phase.
Postoperative pain can be the result of extensive and long surgical procedures; poor tissue handling (including incising with a dull instrument, tissue trauma, and poor local anesthesia); poor infection control (which increases the risk of postoperative infection); or poor knowledge of surgical anatomy (which increases the risk of complications, such as nerve injury and edema).
Presentation
Population
- Patients who underwent:
- Procedures that involved mucogingival or bone structures
- Surgeries with large wounds
- Patients whose healing process might be delayed (e.g., immunosuppressed people, those with uncontrolled diabetes, smokers, those taking bisphosphonates, those with a history of radiotherapy in the head and neck area)
- Patients with a past history of high analgesic intake after periodontal surgery
- Patients experiencing preoperative anxiety
Signs
- Gingival recession
- Gingival inflammation
- Edema (Fig. 1)
- Fever
- Purulent exudate
- Wound dehiscence
- Exposed bone
- Sequestrum
- Ulcers
- Periapical lesions
- Caries
- Root fracture
- Dysesthesia or hyperesthesia
- Sensitivity of area/teeth upon percussion or palpation
- Sensitivity of TMJ or masticatory muscles upon palpation
Symptoms
- Persistent, spontaneous or triggered, localized or diffuse, pain
- Sensitivity to temperature changes
- Edema
- Fever
- “Bad” taste in the mouth
- Difficulty to open the mouth
- Headaches
- Anxiety
Investigation
- Inquire about the patient’s medical and dental history to look for potential etiological factors.
- If another practitioner performed the surgery, contact them and inquire about location, type, difficulty level, and duration of surgery as well as pain management regimen and pertinent medical and dental history.
- Ask the patient about the pain onset, severity, and duration.
- Inquire about the patient’s compliance to postoperative instructions and analgesic intake.
- Verify the amount and dosage of the analgesics taken by the patient for past periodontal surgeries, if applicable.
- Determine with the patient if local factors might trigger the pain (e.g., trauma from brushing or chewing food, temperature stimulus, mouth opening, lying down).
- Perform an intraoral examination to identify potential sources of pain (if pain is unbearable and unmanageable following 3 days of analgesic intake, or if it has increased rather than dissipated since the surgery).
- Assess for the following:
- Presence of postoperative gingival recessions on treated teeth, and if these recessions are sensitive to cold stimulus (air, water), which may lead to a diagnosis of dentinal hypersensitivity (Fig. 2).
- Presence of fever, gingival inflammation, edema, purulent exudate, exposed bone, sequestrum or wound dehiscence in the surgical area or at the local anesthetic injection site, which would likely lead to a diagnosis of infection and/or delayed healing (Fig. 3).
- Presence of ulcers in the surgical area or at the local anesthetic injection site, which may lead to a diagnosis of traumatic or aphthous ulcer, recurrent herpes or herpes zoster (Fig. 4).
- Presence of pulpal or periapical pathologies or caries, or root fracture on treated teeth or teeth adjacent to the surgical area, which may lead to a diagnosis of reversible or irreversible pulpitis.
- Presence of paresthesia or dysesthesia in the surgical area, the surroundings or the injection site, which may lead to a diagnosis of peripheral nerve injury.
- Sensitivity to percussion and radiographic enlargement of the periodontal ligament of teeth involved in the surgical area, which may lead to a diagnosis of trauma from occlusion.
- Pain upon mouth opening, difficulty to open the mouth, masticatory muscles tenderness upon palpation or headaches, which may lead to a diagnosis of TMJ disorder or injury, or trismus.
- Radiographs of the teeth involved in the surgical area and surrounding structures might be necessary if no sources of postoperative pain can be found clinically, or to confirm a diagnosis.
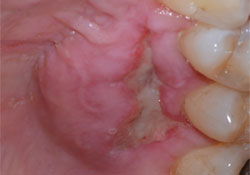 Fig. 1: Edema at a connective tissue graft donor site on the hard palate. This condition is most likely caused by a hematoma.
Fig. 1: Edema at a connective tissue graft donor site on the hard palate. This condition is most likely caused by a hematoma.
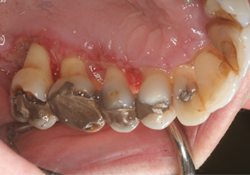 Fig. 2: Dental hypersensitivity caused by root exposure following a periodontal flap surgery for pocket reduction.
Fig. 2: Dental hypersensitivity caused by root exposure following a periodontal flap surgery for pocket reduction.
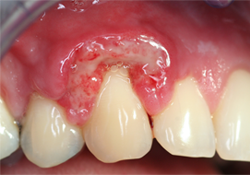 Fig. 3: Delayed healing caused by necrosis of a subepithelial connective tissue graft.
Fig. 3: Delayed healing caused by necrosis of a subepithelial connective tissue graft.
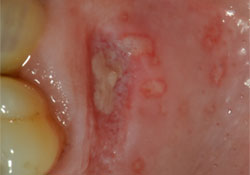 Fig. 4: Recurrent herpetic ulcers at a donor site on the hard palate following the harvesting of a free autogenous gingival graft.
Fig. 4: Recurrent herpetic ulcers at a donor site on the hard palate following the harvesting of a free autogenous gingival graft.
Diagnosis
Based on clinical and radiographic findings (if applicable), a diagnosis can be determined.
Differential Diagnosis
- Dentinal hypersensitivity
- Infection (gingival or periapical abscess)
- Delayed healing (wound dehiscence or necrosis/bone exposure)
- Traumatic or aphthous ulcers/recurrent herpes/herpes zoster
- Reversible or irreversible pulpitis
- Peripheral nerve injury
- Trauma from occlusion
- TMJ injury/trismus
- Individual’s accentuated response to pain
Treatment
Always verify with the patient if they have any known drug allergies or if she is pregnant.
Common Initial Treatments
- If the pain occurs within the first 3 days postoperatively, reassure the patient that pain is normal within that time frame.
- If the pain intensifies after an initial decrease or after more than 3 days postoperatively, or if the pain has been consistently unbearable and unmanageable 3 days after surgery, the diagnosis determines the course of action.
Dental Hypersensitivity
- Reassure the patient that it is a common side effect related to the nature of periodontal surgery, especially pocket reduction surgery.
- Encourage the patient to use a desensitizing agent, such as toothpaste containing potassium nitrate (e.g., Sensodyne®) or arginine and calcium carbonate (e.g., Colgate® Sensitive Pro-Relief™).
- Consider applying a chair-side fluoride varnish or dentinal tubule sealer (e.g., Super Seal®) to help reduce symptoms, if the dentinal hypersensitivity does not go away after 1–2 months.
- Schedule monthly visits until a significant improvement can be seen.
Infection
- Prescribe antibiotics (e.g., amoxicillin 500 mg: 2 tabs stat, then 1 tab t.i.d. for 7 days).
If the patient is allergic to penicillins, prescribe:- Azithromycin 250 mg: 2 tabs stat, then 1 tab q.d. for 4 days; or
- Clindamycin 150 mg: 2 tabs stat, then 1 tab q.i.d. for 7 days; or
- Doxycycline 100 mg: 2 tabs stat, then 1 tab b.i.d. for 7 days.
- Prescribe a 0.12% chlorhexidine gluconate rinse (e.g., Peridex™), used b.i.d. for 30 seconds for 7 days.
- For severe infections with fluctuant swelling, incision and drainage with sterile saline irrigation might be indicated with stronger analgesics, including narcotics in combination with non-narcotics.
- Follow up by phone after 2–3 days. If there is no improvement, consider prescribing an alternate antibiotic.
- In all cases, reevaluate the patient after 1 week.
Delayed Healing
Immediately refer to an oral and maxillofacial surgeon if the complication is associated with bisphosphonate intake or radiotherapy, if the cause is unknown or if there is no improvement 1–2 weeks after the first postoperative control.
- With the patient’s physician, identify potential systemic or medical risk factors.
- If the patient is a smoker, remind them not to smoke as this may cause further delays in healing.
- Ensure the patient’s glycemia is controlled.
- Prescribe antibiotics and 0.12% chlorhexidine gluconate rinse to reduce risks of infection, especially when alveolar bone is exposed.
- Cover the bone with a coronally-positioned flap and/or intracortical perforations with a ¼ round bur and irrigation, to increase the chances a blood clot will form over the exposed bone, thus stimulating epithelialization of the wound.
- Prescribe stronger analgesics, including narcotics in combination with non-narcotics, if needed.
- Reevaluate the patient after 1 week.
Traumatic or Aphthous Ulcers/Recurrent Herpes/Herpes Zoster
- Ask the patient if they have previously experienced ulcers following dental procedures.
- Only palliative treatments are necessary at this point:
- Use of topical anesthetics (e.g., Orajel®) or an analgesic mouth rinse (diphenhydramine [e.g., Benadryl®] 12.5 mg/5 mL mixed with kaopectate), 3–4 times a day until symptoms have subsided
- Use of 0.15% benzydamine hydrochloride rinse (e.g., Tantum®) for 2 minutes, 3–4 times a day, for 1–2 weeks or until symptoms have subsided
- If recurrent herpes or herpes zoster is suspected, prescribe topical acyclovir cream if within 48 hours of symptom onset (acyclovir 5% : apply a thin film on the ulcers 5 times a day for 4 days)
- Reassure the patient that the symptoms should disappear in 7 to 14 days; however, if the diagnosis is herpes zoster, residual pain may be felt for months after the lesions resolve.
- Reevaluate the patient 1–2 weeks later.
Pulpitis
- Advise the patient of the possibility that the surgery might have precipitated the pathology. The pathology could also have been asymptomatically present before the surgery.
- Reversible pulpitis: Eliminate caries or extract the tooth, if the cause is a complicated root fracture.
Irreversible pulpitis: Proceed to endodontic therapy or tooth extraction, if a complicated root fracture is present.
Suspected Nerve Injury
- Determine which sensory structure is involved.
- It is important to precisely document the area and type of sensation felt by the patient (anesthesia, dysesthesia, paresthesia) using specific tests (see suggested resource no. 7).
- Prescribe prednisone (50 mg q.d. for 7 days) as soon as nerve injury is suspected, and reevaluate the patient 1 week later and once a month thereafter.
- Refer to an oral and maxillofacial surgeon if it is not possible to prescribe prednisone or if the symptoms do not improve.
Trauma from occlusion
- Adjust occlusion on the teeth involved in the surgical area that have potentially moved due to local inflammation, only if severe pain persists for more than 3 days.
- Reevaluate the patient 1–2 weeks later to verify occlusion again, as the occlusion might go back to normal spontaneously after resolution of the inflammation.
TMJ Injury or Trismus
- Apply a warm water compress on masticatory muscles and TMJ.
- Advise the patient to avoid hard foods and high amplitude movements.
- Prescribe NSAIDs for the following weeks until reevaluation 2 weeks later.
- Refer to a specialist in oral medicine or an oral and maxillofacial surgeon if the situation does not improve.
Unidentified Source of Pain
- Eliminate potential risk factors that may aggravate the situation.
- Consider prescribing a stronger dose or type of analgesics.
- Reinforce postoperative care instructions.
- A postoperative appointment should be scheduled 1 week later to assess tissue healing and determine if the patient simply had a reduced threshold toward postoperative pain related to anxiety and/or genetics.
Alternate Treatments
If the pain persists after treatment and/or the source of pain remains unidentified, refer the patient to an oral pathologist, specialist in oral medicine, or oral and maxillofacial surgeon to rule out peripheral nerve injury or disturbance, or other pathologies such as cancer and chronic TMJ disorders.
Advice
- Proper treatment planning and management is essential to minimize postoperative pain.
- Always provide verbal postoperative instructions immediately after periodontal surgery and provide detailed written postoperative instructions with emergency contact information to reach the dentist directly.
- A patient’s experience with postoperative pain is difficult to predict and therefore analgesics should be routinely used for consistent pain prevention and management.
- For longer or more extensive periodontal surgeries, NSAIDs and a narcotic combined with a non-narcotic agent are routinely prescribed and will, in most cases, provide acceptable pain management.
THE AUTHORS
Suggested Resources
- Falace, DA. Emergency dental care: diagnosis and management of urgent dental problems. Baltimore: Williams & Wilkins; 1995.
- Hupp JR, Ellis E, Tucker MR. Contemporary Oral and Maxillofacial Surgery. 5th ed. St. Louis: Mosby Elsevier; 2008.
- Rose LF, Mealey BL, Genco RJ, Cohen DW. Periodontics: Medicine, Surgery, and Implants. St. Louis: Mosby Elsevier; 2004.
- Newman MG, Takei HH, Klokkevold PR, Carranza FA. Carranza’s Clinical Periodontology. 11th ed. St. Louis: Elsevier Saunders; 2012.
- Wynn RL, Meiller TF, Crossley HL. Drug Information Handbook for Dentistry. 18th ed. Hudson: Lexi-Comp Inc.; 2012.
- Repchinsky C. Compendium of pharmaceuticals and specialties (CPS); 2012. Ottawa, ON: Canadian Pharmacists Association; 2012.
- Caissie R, Goulet J, Fortin M, Morielli D. Iatrogenic paresthesia in the third division of the trigeminal nerve: 12 years of clinical experience. J Can Dent Assoc. 2005;71(3):185-90.




