Primary Incisor Root Fracture
Injury to a primary incisor following a traumatic injury. Diagnosis of a root fracture may be suspected but must be confirmed radiographically.
Presentation
Population
- Incidence of primary tooth trauma is greatest when motor coordination is developing, around 2–3 years of age.
More Likely to Occur
- Protrusive incisors are more susceptible to dentoalveolar trauma.
- Root fractures are uncommon in the primary dentition. Due to the plasticity of alveolar bone, luxation injuries are more common in the primary dentition.
Signs
- The coronal tooth fragment may be absent, mobile, displaced or display normal physiologic mobility.
Symptoms
- Pain may or may not be reported.
- Inability to occlude or discomfort with occluding if the coronal fragment is displaced or mobile.
Investigation
- Obtain a thorough medical history:
- Note any systemic medical conditions such as bleeding diatheses, compromised immunity, seizure disorders, congenital heart defects, medications, or medicinal allergies that may impact treatment.
- Based upon findings, obtain medical consultations or refer for treatment as appropriate.
- Obtain a thorough dental history, including any history of previous dental or orofacial trauma.
- In case of a traumatic injury:
- Record when, where, and how the accident occurred.
- Inquire if there were any witnesses to the accident.
- Inquire if any treatment was provided prior to arrival at the dental office.
- Perform an extraoral examination:
- Take photographs, if possible, to document injuries.
- Measure and record all wounds using a ruler and/or periodontal probe.
- Palpate maxilla and mandible for signs of fracture.
- Document mandibular range of motion and TMJ tenderness, swelling, clicking or crepitus.
- Palpate and note any neck pain or stiffness.
- Perform an intraoral examination (Fig. 1):
- Take photographs, if possible, to document injuries.
- Measure and record all soft tissue wounds; examine all teeth for traumatic injuries.
- Check occlusion to rule out mandibular fracture.
- Look for pre-existing clinical signs of necrosis (i.e., parulis/fistula).
- Perform a radiographic examination (Fig. 2):
- Occlusal radiograph: position size 2 film and expose as an occlusal film at 60°.
- To confirm presence of a root fracture: additional exposures at different angulations may be required if the coronal fragment is not displaced.
- To rule out or confirm radiographic signs of pre-existing necrosis.
- Occlusal radiograph: position size 2 film and expose as an occlusal film at 60°.
- Soft tissue radiograph(s): ¼ exposure time of a periapical radiograph.
- To rule out foreign matter or tooth fragments in the lips/cheeks if intraoral lacerations are present.
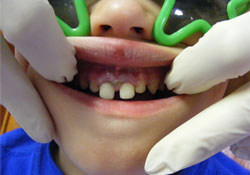 Figure 1: Photograph demonstrating displacement/mobility of the coronal fragments of teeth 51 and 61 following middle third root fractures (see Fig. 2). The coronal fragments were extracted and the root fragments were left in situ.
Figure 1: Photograph demonstrating displacement/mobility of the coronal fragments of teeth 51 and 61 following middle third root fractures (see Fig. 2). The coronal fragments were extracted and the root fragments were left in situ.
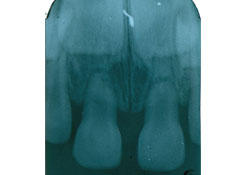 Figure 2: Radiograph taken at the time of trauma by the family dentist prior to referral to the local children's hospital. Neither of the traumatized teeth displayed radiographic signs of pretraumatic caries or necrosis.
Figure 2: Radiograph taken at the time of trauma by the family dentist prior to referral to the local children's hospital. Neither of the traumatized teeth displayed radiographic signs of pretraumatic caries or necrosis.
Diagnosis
Based upon radiographic findings, a root fracture diagnosis is confirmed.
- Occlusal film(s): root fracture visualized, most commonly seen in the middle or apical third
Differential Diagnosis
- Avulsion or complete intrusion, if the coronal fragment is not visible clinically
- Luxation, if the coronal fragment is displaced
- Subluxation, if the coronal fragment is mobile but not displaced
- Concussion, if the coronal fragment is neither mobile nor displaced
Treatment
Initial Treatment
- Immediately refer to an emergency department if any of the following signs/symptoms are present, as these may indicate a head or spinal cord injury:
- Loss of consciousness
- Neck or head pain/stiffness
- Numbness anywhere on the body
- Nausea or vomiting
- Drowsiness or blurred vision
- Perform treatment based on the coronal fragment’s condition.
Coronal fragment is absent- Consider a chest X-ray to rule out aspiration if the coronal fragment cannot be located.
- Do not replant the coronal fragment.
- Leave the apical root fragment to resorb unless:
- the tooth was necrotic prior to the time of injury
- the apical fragment can be easily retrieved
- Extract the coronal fragment.
- Leave the apical root fragment to resorb unless:
- the tooth was necrotic at the time of injury
- the apical fragment can be easily retrieved with forceps/elevators
If the coronal fragment is minimally displaced, International Association of Dental Traumatology guidelines give the option of manual repositioning without splinting
Coronal fragment is not mobile/displays physiologic mobility- No treatment is required, monitor only.
- Suture intraoral lacerations if required.
- Discuss possible sequelae
- Traumatized primary incisor:
- Necrosis: tooth discolouration (not pathognomonic for necrosis), intraoral or extraoral swelling, increasing mobility
- Permanent successor:
- Developmental disturbances (enamel hypoplasia or hypocalcification) are not expected.
Eruption disturbances: delayed eruption or altered eruption path is possible but not expected.
- Developmental disturbances (enamel hypoplasia or hypocalcification) are not expected.
- Space loss in the anterior sextant if the coronal fragment is missing or extracted:
- Maxillary: minimal chance of space loss if the primary cuspids have erupted and anterior arch length is established. Space loss is more likely if the child has an active non-nutritive sucking habit.
- Mandibular: significant chance of space loss unless the tooth was nearing natural exfoliation.
- Traumatized primary incisor:
Follow up
- Coronal fragment absent or extracted
- Clinical and radiographic examinations: annually until the successor erupts
- Coronal fragment displays physiologic mobility or has been repositioned
- Clinical examination: 1-week after injury and then 6–8 weeks after
- Clinical and radiographic examinations: annually until successor erupts
If radiographic signs or clinical signs/symptoms of necrosis or eruption disturbances are observed during the follow-up period, extraction is indicated.
Advice
- Have patient follow a soft diet for 10–14 days and brush with soft toothbrush after each meal.
- Use chlorhexidine (nonalcoholic, if available) twice a day for 1–2 weeks.
- Contact the dental office if pain or signs of necrosis arise between follow-up visits.
THE AUTHOR
Suggested Resources
- Malmgren B, Andreasen JO, Flores MT, Robertson A, DiAngelis AJ, Andersson L, et al. International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: 3. Injuries in the primary dentition. Dent Traumatol. 2012;28(3): 174-82.
- American Academy of Pediatric Dentistry.Policies and Guidelines. Guideline on Management of Acute Dental Trauma [revised 2011; accessed 2013 May 7]. Available:http://www.aapd.org/policies/.
- University Hospital of Copenhagen and the International Association of Dental Traumatology. The Dental Trauma Guide. Primary teeth; Root Fracture [accessed 2013 May 7]. Available:http://www.dentaltraumaguide.org/PrimaryRootfracture_Description.aspx.
- Dean JA, Avery DR, McDonald RE. Chapter 21. In: McDonald and Avery’s Dentistry for the Child & Adolescent. 9th ed. Maryland Heights (MO): Mosby; 2011.
- Casamassimo PS, Fields HW, McTigue DJ, Nowak A. Chapter 15. In: Pediatric Dentistry: Infancy through Adolescence. 5th ed. Elsevier; 2013.
- Andreasen JO, Andreasen FM. Essentials of Traumatic Injuries to the Teeth: A Step-by-Step Treatment Guide. 2nd ed. Oxford (UK): Blackwell Publishing; 2000.

