Author's note: As periodontists, we perform gingival augmentation procedures regularly. On occasion, a treated patient contacts their family dentist following this type of procedure with concerns about the surgical site. Family dentists are also involved in follow-up care, sometimes in the early stages of postoperative healing. The following article is intended to help guide the dentist through concerns they or the patient may have during a follow-up visit.
Presentation
Population
- Individuals with a recent history of gingival augmentation surgery
- Immunocompromised patients and those with delayed wound healing may be at higher risk
Signs
- Dislodged or removed surgical dressing
- Redness of surgical (recipient) site or tissue sloughing
- Approximating vestibular tissue may appear necrotic
- Persistent root exposure likely noted
Symptoms
- Patient may experience pain, described as a constant dull ache or sharper pain during mastication or speaking (movement of oral and peri-oral tissues).
- Patient experiences anxiety over procedure and perceived lack of success.
Investigation
- Perform complete extraoral (head and neck) and intraoral (teeth and soft tissue) exams to rule out postoperative infection. Evidence of postoperative pain, bruising, swelling or even infection does not indicate a gingival graft failure/loss.
- Examine the surgical site:
- Is there evidence of tissue on the periodontal dressing?
- Is there trauma to the site as reported by patient?
- Is there evidence of new tissue covering the periosteum, apical to the tooth or teeth that received the graft?
-
Ascertain which grafting procedure was completed:
- A free gingival graft (FGG) is placed with the goal of increasing the zone of attached gingiva.
- A connective tissue graft (CTG) is placed with the goal of both increasing the zone of attached gingiva and achieving root coverage of a previously exposed root surface.
Diagnosis
Infection
- Severe swelling of localized facial tissues and intraoral site approximating the surgical site
- Localized lymphadenopathy
- Evidence of pus/exudate in the graft recipient site (may be liberated from site with gentle presure)
Surgical Site
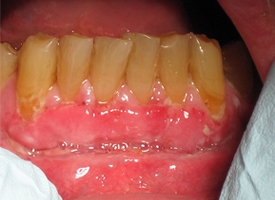
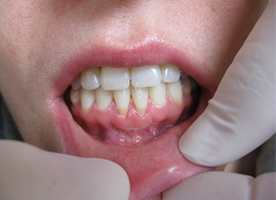
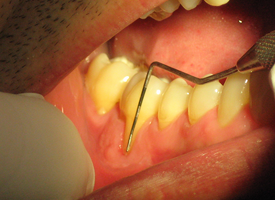
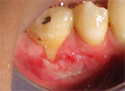
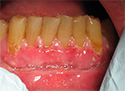
- Dislodged or removed dressing may have evidence of tissue on it. In many instances, this may just be the sloughed epithelium and the remaining connective tissue will have remained/survived at the site (Figs. 1, 2 and 3).
- Most grafting procedures can withstand minor traumas. However, significant traumas (i.e., blow to the face, direct injury to the site with utensil/toothbrush), particularly if occurring in the first 24–48 hours postoperation, can cause graft necrosis.
- Clinical evidence of soft tissue covering periosteum is indicative of graft survival, even in the presence of persistent root exposure.
NOTE: Click to enlarge images.
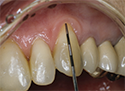
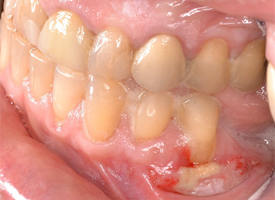 Figure 1: Normal postoperative healing of a free gingival graft. Note "whitish" colour that patients may perceive as "lost graft." (Photo courtesy of Dr. Peter Halford)
Figure 1: Normal postoperative healing of a free gingival graft. Note "whitish" colour that patients may perceive as "lost graft." (Photo courtesy of Dr. Peter Halford)
Graft Type
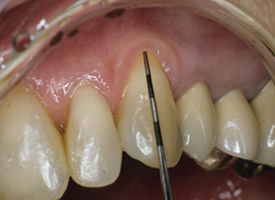
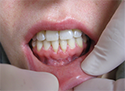
- A successful FGG will show remaining root surface but evidence of healing tissue apical to the exposed root (Figs. 4 and 5).
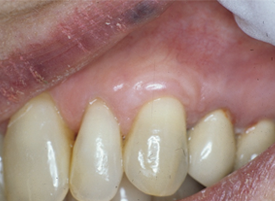
- A successful CTG will have evidence of tissue covering the previously exposed root (Figs. 6 and 7).
Treatment
Common Initial Treatments
Early Stage (<14 days postoperation)
- Reassure the patient.
- Prescribe antibiotic if there is evidence of infection: usually amoxicillin 500 mg, t.i.d. for 3 days is sufficient. Confirm if previous antibiotic has been prescribed and consider alternative drug.
- Pain management: Prescribe anti-inflammatory medication (ibuprofen 400–600 mg t.i.d. or q.i.d. for 4–5 days) or acetaminophen-codeine-caffeine (one tablet q. 4–6h. p.r.n. for 3–4 days).
- Advise the patient to perform minimal or no mechanical brushing of the site.
- Start or continue to use antibacterial mouth rinse for 7–10 days (chlorhexidine 0.12%).
- Contact a periodontist, if required, to advise about your and the patient's concerns.
- Follow up in 21–28 days.
Later Stage (4–6 weeks postoperation)
- Assess root coverage for CTG (may achieve partial coverage of exposed root surface).
- Measure the zone of keratinized gingiva for FGG and CTG.
- If there is no evidence of root coverage (CTG) or of a zone of keratinized gingiva (FGG), retreatment will likely be required. In this instance, contact a periodontist. Success or failure of graft will be determined by the periodontist or the operating surgeon. Failure happens in less than 2% of cases.
THE AUTHOR
| Gallery of all Figures in article | ||||

|
|
|
|
|

|
|
|
||
Suggested Resources
- Parameter on mucogingival conditions. American Academy of Periodontology. J Periodontol. 2000;71(5 Suppl):861-2.
- Greenwell H, Fiorellini J, Giannobile W, Offenbacher S, Salkin L, Townsend C, et al. Oral reconstructive and corrective considerations in periodontal therapy. J Periodontol. 2005;76(9):1588-600.