Body
Mandible fracture during extraction
- Sudden, intra-operative fracture of mandibular bone
Presentation
Population
- Males and patients over age 30
Risk Factors
- Dental anatomy characteristics or anomalies: long or bulbous roots, hypercementosis, and multi-rooted teeth
- Pathoses: cysts, ankylosis, osteoporosis, and alveolar atrophy or, conversely, very dense bone
- Elevator use, particularly large elevators and elevators used as levers, rather than in a rotary fashion
- Impacted teeth requiring bone removal, particularly those that extend to the inferior border of the mandible
Common Sites of Occurrence
- Vertically impacted third molars, close to the inferior border of the mandible, but can occur with other molars (See Figs. 1 and 2).
Signs
- Crunch or loud crack of bone breaking
- Sudden loosening of the tooth or bone
- Bone comes away with tooth during extraction
- Observable malocclusion, opening of the bite, separation of teeth, or step defect
- Radiographic evidence of fracture which may be subtle, non-displaced, or greenstick
Symptoms
- Patient may complain of sharp pain at the time of fracture or may be completely asymptomatic
- Depending on displacement, the patient may be aware of malocclusion
- If the diagnosis is delayed, the patient may return with a complaint of altered sensation in the lip or chin, worsening malocclusion, persistent swelling, persistent pain, or signs of infection (fever, chills, or malaise)
Investigation
Confirm clinical suspicion of fracture and assess displacement
- Gently, with minimal force and movement, assess the degree of mobility across the suspected fracture site.
- Have the patient close into occlusion to assess changes in occlusal pattern.
- Obtain radiographic evidence of fracture with periapical or panoramic radiographs.
- Unless the diagnosis is delayed, assessment of altered sensation in the lip and chin will be masked by local anesthesia.
Diagnosis
- Confirmed mobility of fracture fragments
- Malocclusion
- Radiographic evidence of fracture
- State the displacement of the fracture fragments (none, minimal, moderate, or severe)
Treatment
If possible, the patient should be immediately referred to an oral and maxillofacial surgeon for the management of the mandibular fracture.
-
If the fracture is non-displaced: observation and soft diet may be all that is required.
If the fracture is displaced or unfavourable:- open reduction with plate and screw fixation; or
- maxillomandibular fixation with arch bars or attachment devices using wires or elastic traction
- Advise patient about possible malocclusion, loss of vitality for teeth adjacent to the fracture, infection (including osteomyelitis), and paresthesia.
- Advise patients with difficult extractions to return in 1 week as the majority of fractures associated with extractions are diagnosed either immediately or in the first postoperative week.
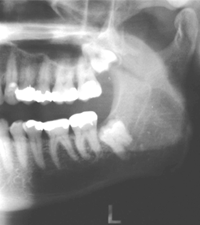 Figure 1: 52-year-old male with pericoronitis associated with a deeply impacted tooth 38.
Figure 1: 52-year-old male with pericoronitis associated with a deeply impacted tooth 38.
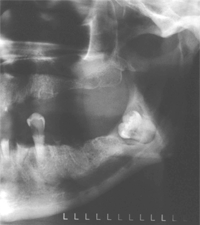 Figure 2: 48-year-old female with bone loss due to pericoronitis around a deeply impacted, carious tooth 38.
Figure 2: 48-year-old female with bone loss due to pericoronitis around a deeply impacted, carious tooth 38.

